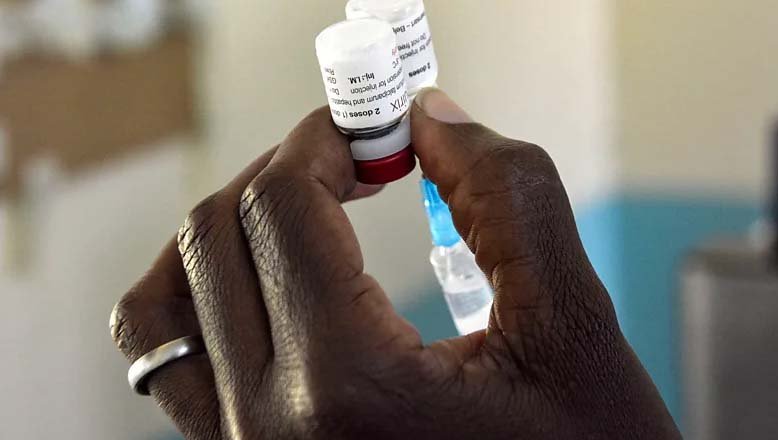
The process of making vaccines for parasites is extremely challenging – but scientists might be on the cusp of major breakthroughs.
There was much celebration in January, when Cameroon became the first country in the world to roll out routine vaccination against malaria. In February, Burkina Faso followed suit.
“Control of malaria has not been going in a good direction, for a lot of different reasons,” explains Kate O’Brien, who directs the department of immunisation, vaccines and biologicals at the World Health Organization (WHO). Malaria cases are rising, and roughly 600,000 people die of malaria each year. Factors include climate change, conflict, the lingering effects of Covid-19 on health systems, and the tenacious adaptability of malaria-carrying mosquitoes. This has meant that the stalwarts of malaria prevention – insecticides sprayed indoors and bed nets treated with insecticides – are losing some of their punch.
Mass malaria vaccination adds one more tool to this package, and one that takes a completely different approach, says O’Brien. “Coming in with an immune-based approach is a very historic and important addition,” she says. In 2019 the RTS,S vaccine against malaria began pilots in Ghana, Kenya and Malawi, and in 2021 the WHO recommended it for use in children. The RTS,S vaccine was followed by the R21 vaccine.
Yet a related milestone has gone less heralded. RTS,S was the first-ever vaccine against a parasitic disease. While diseases caused by parasites are numerous and varied, as a group they are understudied and solutions are underfunded. Most of the neglected tropical diseases, including leishmaniasis and Chagas disease, are parasitic diseases, according to the WHO.
There wasn’t necessarily a concerted effort to make the malaria vaccine the first antiparasitic vaccine. But it’s perhaps unsurprising that it ultimately was, as the high death toll exacted by malaria has led to more attention to developing vaccines for malaria than for other parasitic illnesses (though still not as much as for vaccines affecting wealthy populations, such as Covid-19).
This high mortality rate from malaria makes it a bit of an outlier among parasitic illnesses. Overall, “the death rate from parasitic diseases…is relatively low compared to some other infectious diseases”, O’Brien says. The effects can be disabling and devastating, but not necessarily fatal. Because of this, and because parasitic diseases often are limited to specific parts of low- and middle-income countries, they haven’t been prioritised by conventional vaccine developers.
Peter Hotez is not a conventional vaccine developer. The professor at the Baylor College of Medicine in Houston, who also co-directs the Texas Children’s Hospital Center for Vaccine Development, worked with colleagues to create a late-entrant Covid-19 vaccine that was transferred, free of patent, to vaccine manufacturers in India and Indonesia. At least 100 million doses of the Indian version, Corbevax, have been supplied at approximately $3 (£2.38) per dose. The developers chose an inexpensive vaccine technology: essentially producing a protein in yeast through microbial fermentation. The team are hoping to apply some of the lessons learned from this experience to their work on antiparasitic vaccines, he says.
 Weekly Bangla Mirror | Bangla Mirror, Bangladeshi news in UK, bangla mirror news
Weekly Bangla Mirror | Bangla Mirror, Bangladeshi news in UK, bangla mirror news







