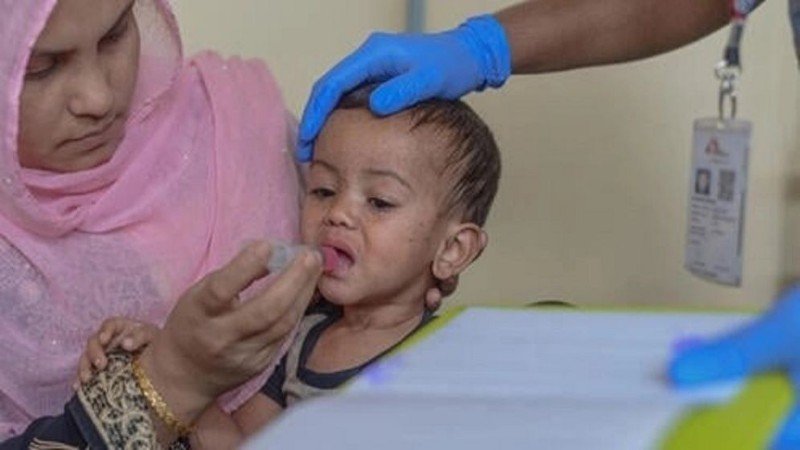
A deepening measles crisis has triggered widespread fear across Bangladesh, with 138 children reported dead and around 9,000 infected as of Sunday.
The outbreak, now affecting 56 districts severely, has raised alarm among families as children continue to succumb to the disease amid an acute shortage of vaccines.
Data and expert analysis suggest that the deaths are linked to systemic failures under the outgoing interim government led by Muhammad Yunus. Allegations include negligence, poor planning, administrative inefficiency and a lack of foresight in ensuring the timely procurement and distribution of vaccines.
Experts and officials point to a series of policy decisions that disrupted the long-standing vaccine procurement system. These include cancelling established supply mechanisms without securing alternatives, failing to allocate sufficient funds from the revenue budget, and not issuing timely directives to ensure vaccine availability. Health sector observers argue that the issue was not treated with urgency by policymakers, leading to the current crisis.
At least 9,000 measles patients are now battling the disease, with public health experts describing the situation as an “epidemic”. They note that gaps in routine immunisation over the past two years have significantly contributed to the rapid spread of the disease.
Sources say the interim government scrapped the existing sector programme—which had been jointly funded by the government and international partners—without adequate preparation. Previously, around 60 per cent of funding came from foreign donors, with the remaining 40 per cent provided by the government. However, after the programme was discontinued in March 2025, no alternative external funding was sought, nor were sufficient domestic allocations ensured.
Criticism has also been directed at former Health Adviser Nurjahan Begum, who is accused of inaction during the unfolding crisis. Public calls for accountability have intensified on social media, with many arguing that policy missteps in vaccine procurement have cost lives.
Health and Family Welfare Minister Sardar Md Sakhawat Hossain told parliament that the absence of measles-rubella vaccination campaigns over the past five and a half years, along with flawed decisions regarding vaccine stock management, had put children at risk.
Public health experts, including Mushtaq Hossain, said efforts to reform the vaccine procurement system were undertaken without adequate preparation, disrupting immunisation programmes and weakening the overall health system. He warned that the government had failed to respond effectively despite early indications of the outbreak.
Another expert, Dr Lelin Chowdhury, noted that although nearly 98 per cent of children were previously covered under routine immunisation, procurement failures during the interim government’s tenure have left a generation of children vulnerable to preventable diseases. He called for an independent investigation to identify those responsible and ensure accountability.
An investigation has also revealed a severe shortage of eight types of vaccines. In the first quarter of this year, only 27.45 per cent of the required measles-rubella vaccine supply was met, leaving more than 72 per cent of demand unmet. Similar shortages were recorded for other essential vaccines under the Expanded Programme on Immunisation (EPI), including pentavalent, oral polio, BCG, inactivated polio, pneumococcal conjugate and tetanus-diphtheria vaccines.
According to EPI Director Shahriar Sazzad, the crisis stems largely from changes in budget allocation and procurement processes. Vaccine purchases were shifted from development to revenue budgets, making fund disbursement more complex and time-consuming.
The suspension of the sector programme has also stalled more than 34 development initiatives in the health sector, disrupting services in primary healthcare, disease control, maternal and child health, and other areas. Experts warn that previously controlled diseases could resurface, while community clinics across the country face shortages of medicines, salaries and essential services.
Professor Benazir Ahmed cautioned that without the continuity of operational plans under the sector programme, health gains achieved over decades could be reversed, potentially increasing child mortality once again. He stressed the need to identify weaknesses, increase funding and sustain long-term public health programmes.
Health experts and stakeholders argue that the decision to scrap the sector programme without adequate study or preparation has had far-reaching consequences. They warn that failure to anticipate the impact of vaccine shortages and ensure timely funding has resulted in a humanitarian crisis, with children paying the ultimate price.
 Weekly Bangla Mirror | Bangla Mirror, Bangladeshi news in UK, bangla mirror news
Weekly Bangla Mirror | Bangla Mirror, Bangladeshi news in UK, bangla mirror news







